Osteoporosis and osteopenia are silent diseases that affect millions of people, especially as they age.
Diet, lifestyle, and certain daily habits play a key role in both their prevention and progression. In this article, we review what happens in the bones, which nutrients help protect them, and which foods should be limited to preserve their strength.
Meritxell Massons – Neolife Nutrition Unit
What Are Osteoporosis and Osteopenia?
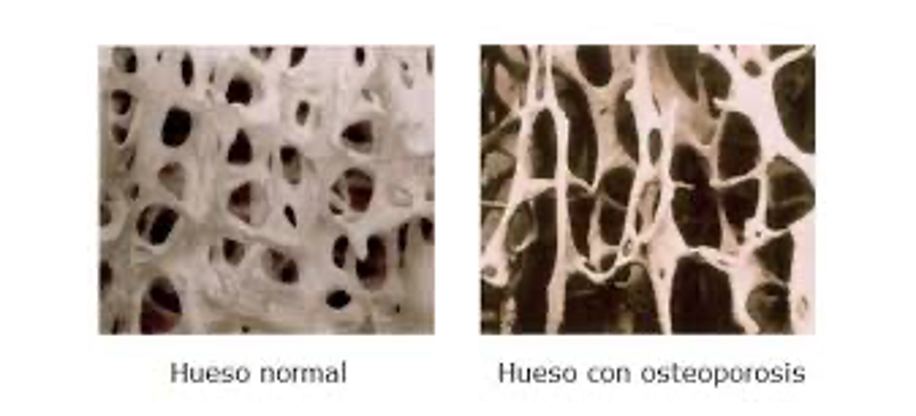
Osteoporosis is a disease characterized by the progressive loss of bone mass and bone quality. The bone becomes more porous and fragile, significantly increasing the risk of fractures, even during everyday activities such as walking or bending down.
Osteopenia is a previous stage in which bone mineral density is lower than normal but does not yet meet the diagnostic criteria for osteoporosis. It is usually detected through a bone densitometry test and represents an important opportunity for prevention.
Why Do Bones Weaken With Age?
Bones are not static structures; they are constantly being renewed. Some cells build bone (osteoblasts), while others break it down (osteoclasts).
- Childhood and adolescence: bone formation predominates.
- Adulthood: a balance is maintained between formation and degradation.
- After the age of 50–60: degradation exceeds formation, especially after menopause due to the decline in estrogen levels.
This process explains why osteoporosis is more common in postmenopausal women and older men.
Preventing Osteoporosis Through Nutrition
Prevention begins long before symptoms appear. Achieving a good peak bone mass during adolescence and early adulthood is essential for long-term bone health.
Calcium: The Structural Basis of Bone
Adequate calcium intake prevents the body from extracting calcium from bones to maintain vital functions such as muscle contraction or blood clotting.
Main sources:
- Dairy products (milk, yogurt, aged and semi-aged cheeses)
- Legumes, nuts, and seeds
- Small fish eaten with bones (such as sardines)
- Vegetables such as broccoli
- Fortified foods (plant-based drinks, cereals)
Two daily servings of dairy products, within a varied diet, usually cover the needs of healthy adults.
Vitamin D: Essential for Calcium Absorption
Vitamin D allows calcium to be properly absorbed in the intestine and deposited in the bone.
Main sources:
- Moderate sun exposure
- Oily fish
- Eggs and dairy products
- Fortified foods
During winter or in individuals with limited sun exposure, deficiencies are common, and supplementation may be necessary under the supervision of a healthcare professional.
Physical Activity: An Essential Stimulus
Exercise, especially weight-bearing activities (walking, climbing stairs, dancing, or strength training), stimulates bone formation. Each muscle contraction sends a positive signal to the bone, helping maintain its density.

Nutrients That Support Bone Health
In addition to calcium and vitamin D, other nutrients play key roles:
- Protein: necessary for the bone matrix, although excessive intake from animal sources should be avoided.
- Magnesium: supports bone mineralization and hormonal activity.
- Zinc: involved in the formation and repair of bone tissue.
- Vitamin C: essential for collagen synthesis.
- Vitamin K: regulates calcium binding in bone.
A varied and balanced diet usually covers these requirements.
Foods and Substances to Limit in Osteoporosis
This does not mean strict prohibitions, but rather moderate and mindful consumption.
- Caffeine
High intake may increase urinary calcium excretion. Limiting coffee, tea, and energy drinks can help protect bone health.
- Excess Phosphorus
Found mainly in soft drinks such as cola and in ultra-processed foods. Excess phosphorus disrupts the calcium–phosphorus balance and negatively affects bone density.
- Alcohol and Tobacco
Both interfere with new bone formation and increase the risk of fractures. Reducing or eliminating them is a key preventive measure.
- Phytates and Oxalates
Present in whole grains, cocoa, coffee, and some leafy green vegetables. It is not necessary to eliminate them, but it is advisable to combine them appropriately and ensure they do not displace calcium-rich foods.
Nutrition and Hormones: A Key Relationship
The loss of estrogen during menopause and testosterone in older men accelerates bone loss. For this reason, osteoporosis is more common in postmenopausal women and in men over the age of 65.
Proper nutrition, together with exercise and medical monitoring, can significantly slow this process.
Conclusion
Taking care of bone health does not depend on a single food, but on an overall lifestyle. A nutrient-rich diet, regular physical activity, and reducing harmful habits are the best tools to prevent osteoporosis and improve quality of life in the long term.
BIBLIOGRAPHY
(1) World Health Organization. Prevention and management of osteoporosis: report of a WHO scientific group. Geneva: World Health Organization; 2003. (WHO Technical Report Series; no. 921).
(2) International Osteoporosis Foundation. Nutrition and bone health [Internet]. Nyon: International Osteoporosis Foundation; 2023 [cited 2026 Feb 9]. Available from: International Osteoporosis Foundation.
(3) National Institutes of Health, Office of Dietary Supplements. Calcium: fact sheet for health professionals [Internet]. Bethesda (MD): National Institutes of Health; 2022 [cited 2026 Feb 9]. Available from: National Institutes of Health.
(4) National Institutes of Health, Office of Dietary Supplements. Vitamin D: fact sheet for health professionals [Internet]. Bethesda (MD): National Institutes of Health; 2022 [cited 2026 Feb 9]. Available from: National Institutes of Health.
(5) European Food Safety Authority. Scientific opinion on dietary reference values for calcium. EFSA Journal. 2015;13(5):4101.
(6) European Food Safety Authority. Dietary reference values for vitamin D. EFSA Journal. 2016;14(10):4547.
(7) Weaver CM, Gordon CM, Janz KF, Kalkwarf HJ, Lappe JM, Lewis R, et al. The National Osteoporosis Foundation’s position statement on peak bone mass development and lifestyle factors. Osteoporosis International. 2016;27(4):1281–1386.
(8) Bonjour JP. Protein intake and bone health. Int J Vitam Nutr Res. 2011;81(2–3):134–142.
(9) Rizzoli R, Biver E, Brennan-Speranza TC, Bilezikian JP. Nutritional intake and bone health. Lancet Diabetes Endocrinol. 2021;9(9):606–621.


