The percentage of men with osteopenia between 35-50 years is higher than that of women. A study done in the southern United States showed that 28% of men and 26% of women had femoral neck osteopenia.
In another study of 173 men and women, exercise and Body Mass Index (BMI) showed an inverse relationship with Bone Mineral Density (BMD). These findings surprised researchers who didn’t expect low BMD to be more common in men than in women.
Dr. Alfonso Galán González – Neolife Medical Team
Osteoporotic fractures are a real health problem.
It is estimated that mortality in the first year after suffering an osteoporotic hip fracture is 30%. Moreover, among those who don’t die, only 20% return to their pre-fracture condition and a large portion need to be fully admitted for care.
Osteopenia can lead to osteoporosis. Osteoporotic fractures are a real health problem. In the United States alone they cause 500,000 hospitalizations and 800,000 ER visits a year and lead to significant rates of mortality. It is estimated that mortality in the first year after suffering an osteoporotic hip fracture is 30%. Moreover, among those who don’t die, only 20% return to their pre-fracture condition and a large portion need to be fully admitted for care (2).
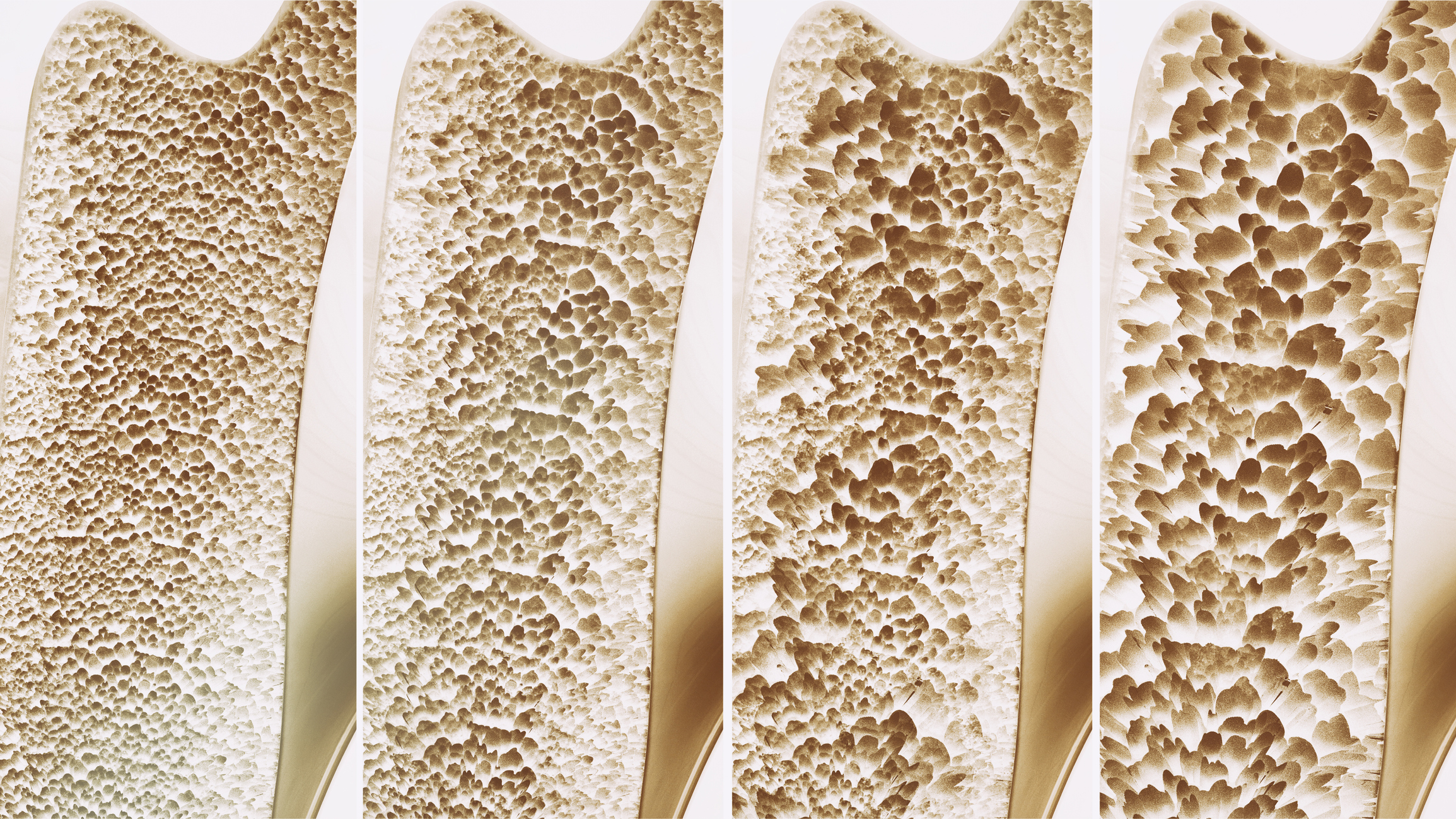
Nutrition, lifestyle, environment, physical activity, and genetics contribute to BMD and it is believed that BMD peaks for individuals in their 30s. Performing weightlifting exercises, running, jumping, etc. helps maintain the BMD. In fact, in this study many of the men studied had strong exercise habits, but cycling and swimming were their sports of choice.
The risk factors for osteopenia are well-studied in older populations but not in middle-aged adults. We can classify these factors as:
- Modifiable: Sedentary lifestyle, low BMI, use of steroid drugs, smoking, excessive drinking, low calcium consumption, low sun exposure, use of antidepressants and antacids, etc.
- Not modifiable: Age, sex, race, etc.
Male hypogonadism causes decreased BMD and is related to increased risk of fracture. Hormone Replacement Therapy with testosterone can effectively reverse the loss of bone due to this cause in men by lowering bone remodeling and increasing trabecular density (3). In addition, multiple studies indicate that it decreases subcutaneous fat and increases the muscle mass helping to reduce the risk of fractures (4).
DHEA (Dehydroepiandrosterone), an adrenal hormone that has been widely discussed in other issues of this newsletter, on the other hand, also has beneficial effects on bone metabolism. The decrease in DHEA levels over the years is closely related to changes in different tissues occurring over time.
Thus, a study in which men and women aged 73 to 75 were supplemented with 50 mg of DHEA for 6 months showed an increase in BMD, muscle mass, IGF-1 (hormone that regulates the anabolic effects of the growth hormone) and testosterone levels and a decrease in fat mass (5).
At Neolife we take care of your bone health and use the Hormone Replacement Therapy with bioidentical hormones to improve your current and future condition.
BIBLIOGRAPHY
(1) Bass MA, Sharma A, Nahar VK, Chelf S, Zeller B, Pham L, Allison Ford M. Bone Mineral Density Among Men and Women Aged 35 to 50 Years. J Am Osteopath Assoc 2019;119(6):357–363.
(2) https://isanidad.com/106692/la-mortalidad-en-el-primer-ano-tras-una-fractura-de-cadera-en-pacientes-con-osteoporosis-es-el-del-30/
(3) Golds G, Houdek D, Arnason T. Male Hypogonadism and Osteoporosis: The Effects, Clinical Consequences, and Treatment of Testosterone Deficiency in Bone Health.
Int J Endocrinol. 2017;2017:4602129. doi:10.1155/2017/4602129
(4) Katznelson L, Finkelstein JS, Schoenfeld DA, Rosenthal DI, Anderson EJ, Klibanski A. Increase in bone density and lean body mass during testosterone administration in men with acquired hypogonadism. J Clin Endocrinol Metab. 1996 Dec;81(12):4358-65.
(5) Villareal DT, Holloszy JO, Kohrt WM. Effects of DHEA replacement on bone mineral density and body composition in elderly women and men. Clin Endocrinol (Oxf). 2000 Nov;53(5):561-8.

