Flu vaccines aim to reduce influenza-related mortality and morbidity and the spread of the disease through the community. Therefore, it is aimed at protecting people who are at higher risk of complications in the event of catching the flu.
People who have received previous influenza vaccines may show a lower severity in COVID-19 due to the immune response induced by the effect of the influenza virus, which, in turn, could react against SaRS-CoV-2.
Dr. Alfonso Galán González – Neolife Medical Team
For decades, the most developed countries have recommended influenza vaccination for the elderly, and this recommendation is also expanding to developing countries. However, recently, it has been criticized due to a perception of poor effectiveness.
On this blog post, we will address the role of the influenza vaccine in the midst of the COVID-19 pandemic, is it necessary or not? Does it help? Does it do any harm? As always, we will see what science has to say to solve doubts.
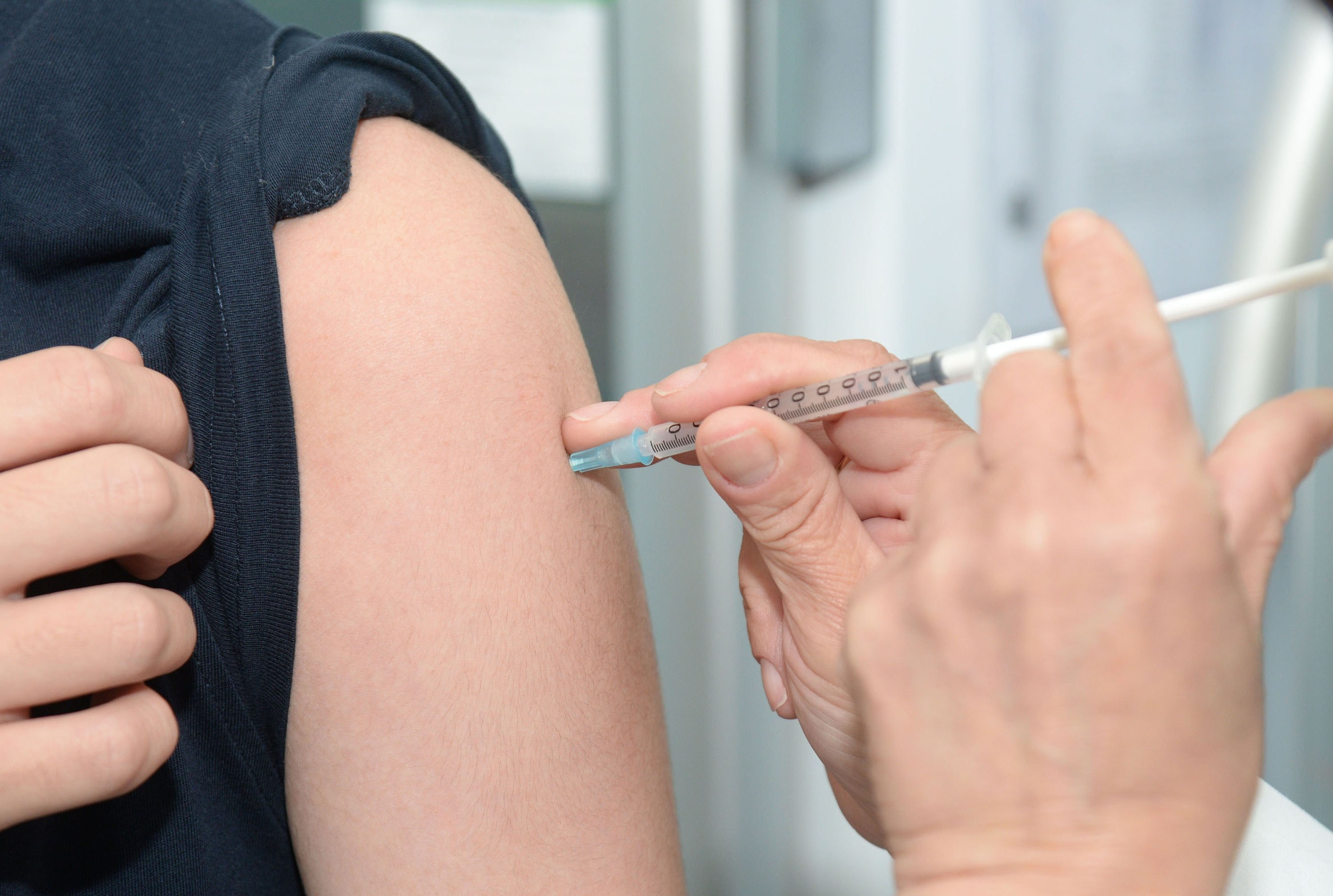
Influenza vaccination
First of all, let’s speak a bit about the flu vaccine (influenza) that health authorities recommend for this season.
Each February, the WHO publishes the composition of the vaccine to be used in the Northern Hemisphere.
The recommended trivalent vaccines for the 2020-2021 season, according to this document, should contain the following components:
Those produced by embryonic eggs and live attenuated vaccines:
- A/Guangdong-Maonan/SWL1536/2019 (H1N1)pdm09 analogue strain
- A/Hong Kong/2671/2019 (H3N2) analogue strain
- B/Washington/02/2019 (B/Victoria line) analogue strain
Those produced from cell cultures:
- A/Hawaii/70/2019 (H1N1)pdm09 analogue strain
- A/Hong Kong/45/2019 (H3N2) analogue strain
- B/Washington/02/2019 (B/Victoria line) analogue strain
In addition to the above, tetravalent vaccines must contain a B/Phuket/3073/2013 (B/Yamagata/16/88 line) analogue strain.
Flu vaccines aim to reduce influenza-related mortality and morbidity and the spread of the disease through the community. Therefore they should be primarily aimed at protecting people who are at higher risk of complications in the event of catching the flu and those who can transmit the disease to others who are at high risk of complications. In summary, and to avoid listing all of the population groups for which it is recommended, we will say that it’s recommended for:
- Older population, preferably people over 65 years of age.
- People under 65 years of age who are at high risk for flu-related complications: Children (from 6 months) and adults with chronic cardiovascular, neurological or respiratory diseases such as: diabetes, morbid obesity, chronic kidney disease, anemia and coagulation disorders, neuromuscular diseases, immunosuppressed people, cancer patients, pregnant women…
- People who can spread the flu to those at high risk of complications: health care professionals, people working at nursing homes, people providing at-home care to high-risk or elderly patients.
- Other groups where vaccination is recommended: state security forces, fire fighters, prison staff, etc.
- It is also recommended for people with direct occupational exposure to domesticated birds or pigs, at poultry or pig farms. The goal is to reduce the chance of a concomitant infection of human and avian/porcine viruses, reducing the possibility of any recombination of genetic exchange between both viruses.
The World Health Organization (WHO) estimated that the influenza virus infects between 5 and 15% of the population each year. The estimated global burden of influenza is nearly 1 billion people infected, to 3 to 5 million cases of severe illness, and between 250,000 and 500,000 deaths. Most influenza-related deaths in developed countries occur among people over 65 years of age, or older. According to data from the European Center for Disease Prevention and Control (ECDC), seasonal influenza causes between 40 and 50 million symptomatic cases each year in the European Union (EU), and between 15,000 and 70,000 people die from the after-effects of influenza.
The main goal of vaccination is the prevention of serious infections, complications, hospitalizations and, ultimately, death; this is especially important among high-risk groups such as the elderly. For decades, the most developed countries have recommended influenza vaccination for the elderly, and this recommendation is also expanding to developing countries. However, recently, it has been criticized due to a perception of poor effectiveness.
The aim of this article isn’t discussing the effectiveness or not of this public health strategy, we will only echo the main problem that appears due to these criticisms. A Cochrane meta-analysis back in 2010 on immunization trials concluded that flu vaccines do not offer any benefits. The European Scientific Working Group on Influenza (ESWI) quickly refuted the Cochrane findings, stating that any doubts on the benefits of influenza vaccination are both scientifically and ethically dangerous. Specifically, ESWI nots that the Cochrane Review was unable to distinguish between seasons with high, mild, or no circulation of an influenza virus, a factor that would dramatically influence any effectiveness estimate.
The current media discussion is based on a dramatic misinterpretation of 2 scientific notions: the efficiency and effectiveness of influenza vaccines. Effectiveness studies measure the level of protection offered by the influenza vaccine against influenza-like diseases. However, it is common scientific knowledge that influenza vaccines offer no protection against other viruses other than the circulating influenza viruses.
Efficacy is more specific to the influenza virus, however, efficacy studies require thorough laboratory research. When data are stratified by risk, a rigorous analysis yields substantial evidence in favor of the flu vaccine to reduce the risk of influenza infection and influenza-related illness and death in the elderly.
Influenza vaccine and COVID
Well, what about COVID? What is the relationship between influenza vaccination and the novel coronavirus?
The scientific community had, at the beginning of the summer, to draft a document under the title “Possible cause of the coronavirus pandemic: Immune interference between adjuvated influenza vaccine POLYSORBATE 80 and SARS-CoV-2”, which related the poor evolution of SARS-CoV-2 infections with prior exposure to the influenza vaccine.
This study has been criticized for having serious methodological defects and it seems to be proven that the effect is quite the opposite.
Thus, we will mention two studies that show an association between influenza vaccination and “protection” against COVID-19.
A study, published by Labin et al. in July 2020 suggests that the resulting immunity against a previous influenza infection would, at least in part, promote immunity against SARS-CoV-2. This hypothesis is based on similarity in quality immunity to both viruses and in previous studies showing cross-reactivity between influenza and the novel coronavirus, became of the similarity between their structures. It is also possible that people who have received previous influenza vaccines may show a lower severity in COVID-19 due to the immune response induced by the effect of the influenza, virus, which, in turn, could react against SaRS-CoV-2.
Another study provided statistical evidence of an association between the increase of influenza vaccinations in Italy and a drop in COVID-related deaths. There may be several explanations for this association observed. One, that the influenza vaccine stimulated innate immunity so that when another respiratory pathogen, such as COVID emerged, the immune of the lung would be prepared for a rapid response and that could affect catching SARS‐COV-2 or the course of COVID-19. Another explanation of the association could be that the adoption of the influenza vaccine could occur in higher economic groups, who had better overall health, or that this association is due to chance. Clearly, further studies are needed to confirm whether this association is really a causal relationship, that is, that influenza vaccination is the cause of the lowest COVID-19 mortality in older people.
Considering this, we could at least say that, at best, it confers protection, and at worst, it bears no relationship, but it’s not an issue, so to speak.
What we need to take into account is that due to the fact that the influenza vaccination affects the number of infections, severe course, hospitalizations and death from the influenza virus, the burden on the healthcare system will be lower and will allow us to have more resources to care for those infected by COVID-19.
BIBLIOGRAPHY
(1) Jefferson T, Di Pietrantonj C, Al-Ansary LA, Ferroni E, Thorning S, Thomas RE. Vaccines for preventing influenza in the elderly. Cochrane Database Syst Rev 2010; (2); PMID:20166072;
(2) Smetana J, Chlibek R, Shaw J, Splino M, Prymula R. Influenza vaccination in the elderly. Hum Vaccin Immunother. 2018;14(3):540-549. doi:10.1080/21645515.2017.1343226
(3) Koutsakos M., Wheatley A.K., Loh L., Clemens E.B., Sant S., Nüssing S. Circulating TFH cells, serological memory, and tissue compartmentalization shape human influenza-specific B cell immunity. Sci Transl Med. 2018;10(428):1–15.
(4) Zheng J., Perlman S. Immune responses in influenza A virus and human coronavirus infections: an ongoing battle between the virus and host. Curr Opin Virol. 2018(28:42):52.
(5) Zeng Q., Langereis M.A., van Vliet A.L.W., Huizinga E.G., de Groot R.J. Structure of coronavirus hemagglutinin-esterase offers insight into corona and influenza virus evolution. Proc Natl Acad Sci. 2008;105(26):9065–9069.
(6) Marín‐Hernández, D., Schwartz, R.E. and Nixon, D.F. (2020), Epidemiological evidence for association between higher influenza vaccine uptake in the elderly and lower COVID‐19 deaths in Italy. J Med Virol.
(7) https://www.mscbs.gob.es/profesionales/saludPublica/prevPromocion/vacunaciones/docs/Recomendaciones_vacunacion_gripe.pdf
