Aging, as we all know, is a set of processes that lead to the deterioration of the body over time. Today, we will talk about the role of inflammation.
Old age is associated with the development of chronic systemic (affecting the whole body) low-grade inflammation on a sustained basis. The term “inflammaging” is often used. This inflammaging state contributes to the onset of age-related diseases such as muscle wasting (sarcopenia) and frailty.
Dr. Celia Gonzalo Gleyzes – Neolife Medical Team
Inflammation Mechanisms
Acute inflammation is the set of processes that appear as a response to tissue damage in the body; this may be related to an external pathogen.
The aim of this mechanism is to limit microbial infection and repair damaged tissues.
An inflamed area is characterized by neutrophil extravasation. These cells are granulocyte-type leukocytes, and they contain lytic enzymes and phagocytin (a substance with antibacterial effects).
After extravasation, neutrophils and other inflammatory cells die in a programmed manner (called apoptosis), so their remains are captured (called phagocytosis) by macrophages (immune system cells derived from monocytes) to resolve the inflammation and return to tissue homeostasis.
This phagocytosis by macrophages is called “spherocytosis”. This is necessary because otherwise, apoptotic neutrophils could release molecules that are harmful to the tissue causing damage. Spherocytosis would also limit unnecessary extravasation of neutrophils once the pathogen is neutralized. In this way, the inflammation would be effective and self-limited over time.
Altered inflammation in aging
With age, the mechanisms that regulate inflammation are altered, and this has an impact in two ways: increased risk of infections and susceptibility to chronic diseases.
An increase in circulating inflammatory mediators (cytokines) is observed in the absence of infection, suggesting the presence of a chronic low-grade inflammatory state. A sustained inflammation will cause tissue damage and consequently pathologies such as atherosclerosis and dementia.
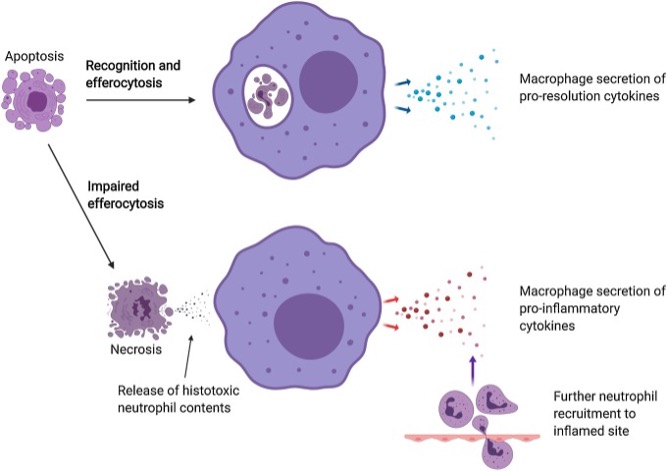
Dysfunction of certain processes due to aging
Neutrophils in older individuals would have a lower response to antiapoptotic stimuli. It is currently being investigated whether chemotaxis, attraction of the macrophage by the neutrophil, may be altered with age; further studies are still required to confirm this. Others point to an altered spherocytosis or a lack of monocyte maturation.
Macrophage polarization is another important point. The normal pathway would be for a macrophage to initiate spherocytosis and secrete anti-inflammatory interleukins to terminate the process. The opposite would be to have macrophages in the injured tissue that worsen the problem (secretion of inflammatory interleukins).
Polarization to a macrophage pro-resolving phenotype has been found to be induced by specialized pro-resolving mediators (SPMs), a superfamily of bioactive substances synthesized from essential fatty acids. SMPs include lipoxins, resolvins, protectins, and maresins. Again, it is possible that aging alters the biosynthesis of SMPs.
Conclusions and new horizons
Inflammaging may be understood as the combination of the inappropriate onset of inflammation and the poor resolution of inflammation, all linked to aging.
As for possible therapies to treat these problems, the usefulness of statins (3-hydroxyl-3-methylglutaryl coenzyme A inhibitors) is being studied. Lovastatin has been shown to enhance spherocytosis in alveolar macrophages in patients with chronic obstructive pulmonary disease (COPD), a pathology characterized by chronic inflammation of the lungs.
Another line of research involves modulating treatments of SPMs to promote the resolution of inflammation. (1)
BIBLIOGRAFÍA
(1) Sendama W. The effect of ageing on the resolution of inflammation. Ageing Res Rev. 2020 Jan;57:101000. doi: 10.1016/j.arr.2019.101000. Epub 2019 Dec 17. PMID: 31862417; PMCID: PMC6961112.
(2) https://pubmed.ncbi.nlm.nih.gov/31862417/#:~:text=Abstract,such%20as%20sarcopenia%20and%20frailty