It is estimated that 50% of adult women may have some degree of urinary incontinence, but only some of them will be diagnosed and treated.
Urinary leaks are bothersome and affect a woman’s quality of life. But no woman should give up hope. There are several solutions to this problem. The starting point is the formulation of an adequate diagnosis.
Dr. Celia Gonzalo Gleyzes – Neolife Medical Team
The health impact of urinary incontinence (UI)
- Quality of life: UI is associated with depression, anxiety, work problems, and social isolation. It also increases the degree of dependency and care.
- Sexual dysfunction: one third of people with incontinence present it during sexual activity, having a negative impact on it (lower frequency and poor quality).
- Morbidity: increased risk of infections (candida or cellulitis due to maceration and irritation) and falls (in urge incontinence and slips).
- Increase in the need for care and degree of dependency: in the United States, it is estimated that up to 10% of nursing home admissions are due exclusively to the problem of UI.
Epidemiology and risk factors
More than 50% of women over the age of 65 may be affected by urinary incontinence. In certain cases, urinary incontinence can be resolved.
The following are factors that contribute to the development and persistence of urinary incontinence.
- Age: the prevalence and severity of UI increases with age.
- Obesity: is a major risk factor for UI. In people with obesity, the risk is tripled. Losing weight can improve or solve the problem (especially in stress incontinence).
- Childbirth: the number of births increases the risk of UI, however, women who haven’t given birth may also have UI.
- Type of delivery: Vaginal delivery increases the risk of stress UI; however, a C-section does not prevent UI in general.
- Family history: there is a genetic component to urge urinary incontinence.
- Other: smoking, caffeine intake, diabetes, stroke, depression, fecal incontinence, menopausal genitourinary atrophy, genitourinary surgery, and radiotherapy treatments.
Types of urinary incontinence
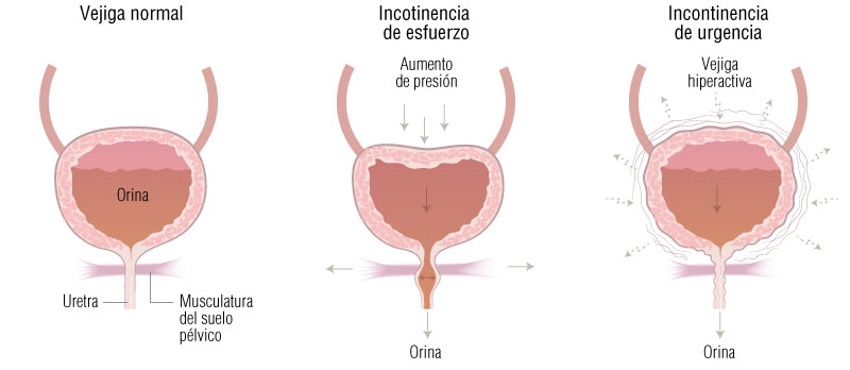
It is essential to know what problem we are facing to guide the therapeutic response. Women may present one type of urinary incontinence or sometimes overlap several.
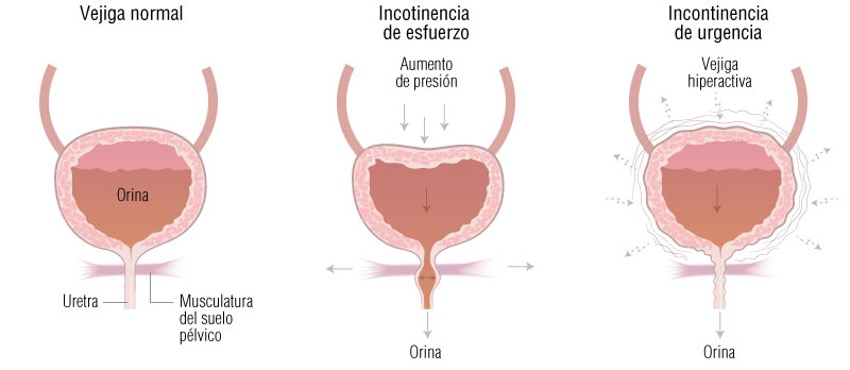
- Stress urinary incontinence: urinary leaks occur when intra-abdominal pressure increases, i.e., when laughing, coughing, sneezing, carrying weight, or during physical exertion.
It is more frequent in women under 60 years of age. The problem lies in the urethral sphincter or in the structures that support it (pelvic floor).
- Urge urinary incontinence: there is an “uncontrolled” activity of the bladder (detrusor muscle) resulting in a sudden urge to urinate. It affects older women.
- Overflow urinary incontinence: the activity of the detrusor muscle decreases. There may also be an obstruction in the outlet (external compression of the urethra), resulting in poor emptying of the bladder. The causes are very varied: fibroids, prolapse, cancer, neurological problems…
Contributing factors to UI include: genitourinary atrophy (due to low estrogen levels at menopause), urinary tract infections, genitourinary fistulas, neurological problems, cancer, some medications, constipation, alcohol and caffeine consumption, dependence, and cognitive problems.
Diagnosis
We will not detail the diagnostic protocol because it includes numerous steps and tests. The first thing you should do is consult with a general practitioner, who in turn will refer you to another specialist, for example, a gynecologist, urologist (for women), neurologist, oncologist, or hormone replacement therapy specialist.
Available treatments for urinary incontinence
Review hygienic dietary measures:
- Control weight with the help of a dietician; treat obesity
- Limit toxic substances: alcohol, smoking, and caffeine
- Fractionate daily water intake
- Adapt physical activity: limit certain activities (CrossFit and abdominal crunches), perform complementary exercises for the perineum (yoga, Pilates), etc.
Ensure protection and hygiene:
Use special pads for urine leaks to be able to continue leading a normal life (avoid social isolation for fear of leaks), to avoid skin maceration, dermatitis and the risk of urinary tract infections.
Kegel exercises:
They are useful in stress and urge incontinence (they facilitate the inhibition of detrusor muscle contractions).
It is necessary to do 3 sessions per day (voluntary contraction of the perineum); each session includes 3 series of 8-12 sustained contractions (8-10 seconds).
Weighted vaginal cones:
The goal is to retain the cone so that it doesn’t fall, strengthening the pelvic floor muscles.
Perineal biofeedback:
This is a vaginal pressure sensor with audible activation. Sometimes you can attach an electrical stimulation system to help the muscles contract.
Hormone replacement therapy:
Undoubtedly, estradiol can combat the urogenital atrophy that is typical in menopause. The hormonal treatment improves the blood flow in that area, among other things.
It is useful in stress and urge incontinence.
Mid-urethral sling:
A minimally invasive surgical technique, a band of synthetic material is placed to support the urethra.
The results are usually good (used in stress incontinence).
Pharmaceutical treatment:
- Botulinum toxin A
- Anticholinergics in urge UI
- Duloxetine, a serotonin and norepinephrine reuptake inhibitor (for urge UI)
Other techniques:
- Transurethral treatments with radiofrequency
- Intravesical balloons
- Electric acupuncture
- Stimulation of some nerves at the sacral level (1, 2, 3)
Practical tips:
If there are signs of the beginning of urinary incontinence, take action.
First and foremost, there should be prevention. If you are approaching menopause, look for a center specialized in bioidentical hormone replacement therapy, like Neolife.
Modify your lifestyle (review dietary and hygienic measures).
If your urinary incontinence is accompanied by other symptoms (weight loss, bleeding, pain), see your doctor promptly.
BIBLIOGRAFÍA
(1) Evaluation of females with urinary incontinence. uptodate.com
(2) Treatment of urinary incontinence in females. www.uptodate.com
(3) NICE guidelines.