It is common knowledge that hygiene allows us to prevent disease. Self-care is defined by the individual’s concern for their health and the measures they put in place to ensure it. “Altered” gums could be the cause of serious illness.
Periodontal disease affects supportive dental structures such as the gums, the cement, the periodontal ligament, and the alveolar bone. It is a condition with a high prevalence in the population and may be related to dementia, oral/colorectal cancer, cardiovascular disease, diabetes, respiratory infections, and complications during pregnancy.
Dr. Celia Gonzalo Gleyzes – Neolife Medical Team
Classification of periodontal disease
This pathology is classified according to the presence or absence of involvement of the periodontal ligament or/and alveolar bone:
- Gingivitis: it only refers to the inflammation of the gums; these may be red, they may bleed or be painful.
- Periodontitis: there is gingival (gum) inflammation that is accompanied by a loss of supportive connective tissue (periodontal ligament and alveolar bone). Clinically, bleeding is observed when the probe is inserted into the gum; it is inserted more deeply than in a normal situation; the teeth may have some abnormal mobility. On the x-ray, depending on the degree of severity, we may observe bone loss (1).
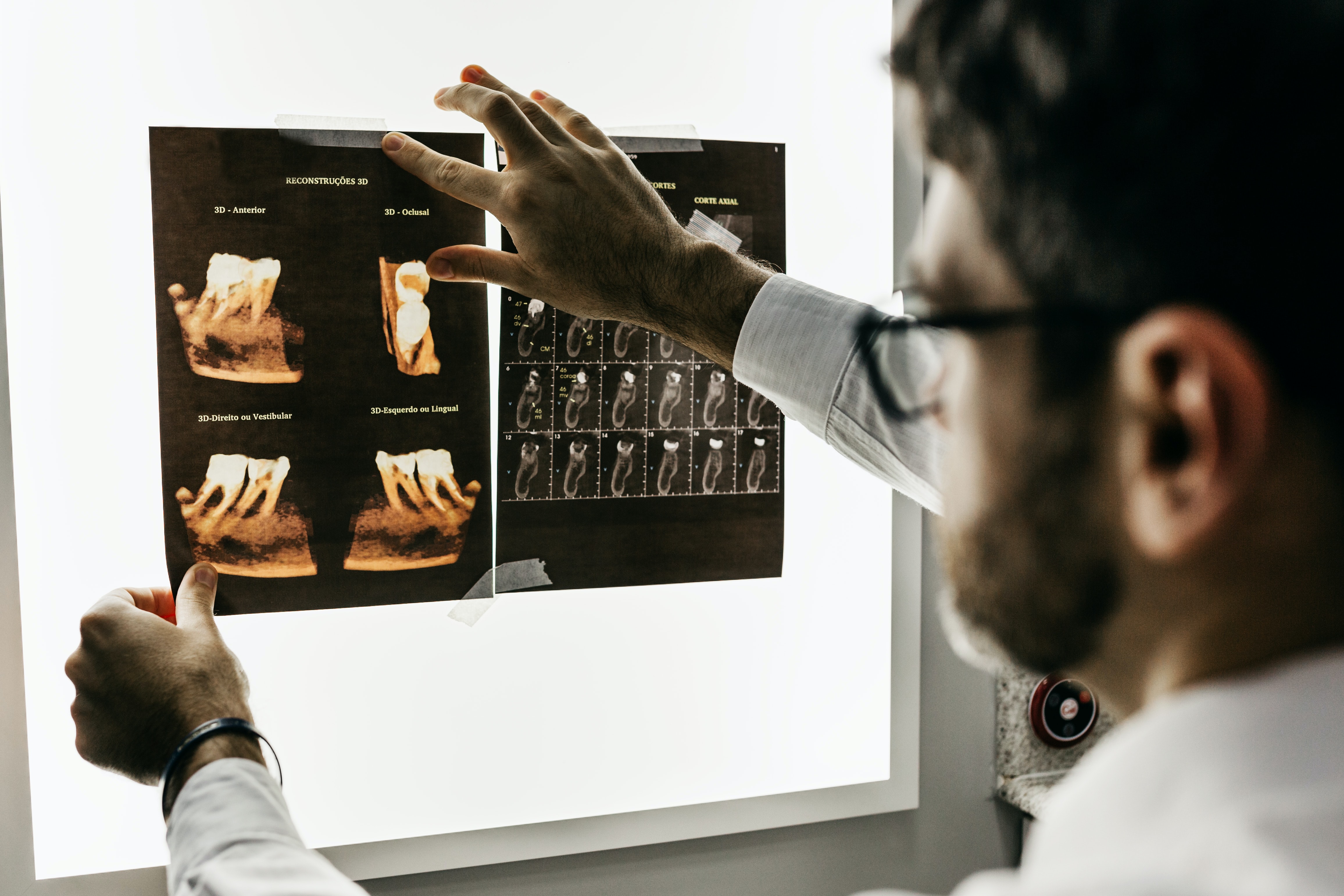
Dental plaque, responsible for this process
The most common gram-negative bacteria in the oral cavity include: Treponema, Bacteroides, Porphyromonas, Prevotella, Capnocytophaga, Peptoestreptococcus, Fusobacterium, Actinobacillus, and Eikenella.
The oral microbiota is present in the saliva, the gingival epithelium, and other surfaces of the oral cavity but is concentrated in the plaque. Dental plaque is a biofilm (it includes a gel-like matrix) made up of microorganisms that are attached to each other and to the dental surface. These characteristics allow them to survive and to resist their hosts defenses and antibiotics. With biofilm maturation a dysbiosis occurs. Gram-positive bacteria are replaced by anaerobic gram-negative ones (responsible for halitosis among other things) and plaque spreads under the gums. The metabolization of sugar by the biofilm of dental plaque promotes the production of organic acids leading to a lowering of the pH and the demineralization of the dental surface. Chewing, normal brushing, and even the use of dental floss in these patients with plaque may cause ruptures of small blood vessels that allow the bacteria to spread through the bloodstream.
Other causes of periodontal disease that we will not address here are: peri-implantitis, pregnancy gingivitis, linear gingival erythema, vitamin C deficiency (scurvy), drug-induced gingival overgrowth, gingival recession, and abscesses.
Systemic diseases related to periodontal disease
This problem will not only cause discomfort and lead to the loss of teeth, but it may also be associated with serious pathologies, caused by the widespread inflammation and the spread of bacteria.
1-Cardiovascular disease
Several studies have shown that the prevalence and incidence of cardiovascular disease increased in patients with periodontitis. The number of teeth is significantly related to the risk of heart attack (the lower the number, the higher the risk).
Bacterial genetic material (DNA) has been confirmed in atheromatous plaque removed by endarterectomy. The most frequently identified bacterium was P.gingivalis, a typical pathogen in the oral cavity. It has the ability to evade the innate immune system by facilitating vascular inflammation, and may add platelets (risk of thrombosis).
Measuring P.gingivalis in saliva could be a marker of cardiovascular risk (2).
2-Respiratory infections
Lung infections may be caused by bacteria, fungi, viruses, and parasites. Microorganisms can infect the lower respiratory tract when we inhale infectious aerosols and by the spread of contiguous or extrapulmonary infections.
The oral cavity (saliva and plaque of patients with periodontal disease) is a source of bacteria, and many of these have been the cause of respiratory infections.
Another interesting fact: individuals with periodontitis are three times more likely to develop nosocomial (hospital-acquired) pneumonia compared to those who do not have this dental problem.
F.nucleatum and F.necrophorum, both oral pathogens, cause Lemierre syndrome (pharyngitis that results in respiratory infection).
C. pneumoniae is thought to pass from the oral cavity to the lungs (common COPD infection, asthma, and bronchitis) to eventually spread through the blood stream, eventually increasing the risk of atherosclerosis.
3-Oral and colorectal cancer
A meta-analysis that included 3183 individuals showed that patients with periodontal disease had an increased risk of oral cancer. Others correlated periodontal disease with pancreatic, head and neck, and lung cancer. Moreover, P.gingivalis has been detected at elevated levels in epidermoid cancers.
P.gingivalis and F.nucleatum stimulate tumor growth through the direct interaction with epithelial oral cells.
As for colon cancer, it is speculated that oral F.nucleatum can migrate and colonize the digestive tract, causing infection and inflammation, and thus contributing to neoplastic progression.
4-Diabetes mellitus
Periodontal disease acts as an infectious disease that causes inflammation and consequently increased insulin resistance, worsening blood sugar control in diabetics, increasing insulin requirements and glycemic variability.
The relationship is bidirectional, meaning that people with diabetes are at higher risk of developing periodontal disease.
5-Alzheimer’s disease
It is a neurodegenerative disease characterized by irreversible alterations in memory, language, and cognitive abilities, which ultimately leads to individual’s death. Beta-amyloid plaques are formed, which are toxic to synapses, and tau proteins are hyperphosphorylated.
Inflammation would be the link between Alzheimer’s disease and periodontal disease.
An increase in pro-inflammatory cytokines has been detected in elderly patients with Alzheimer’s disease and periodontitis.
On the other hand, in the brains (post-mortem) of patients with Alzheimer’s disease, the presence of the bacteria P.gingivalis and T.denticola has been identified.
6-Complications during pregnancy
Because of hormonal changes, pregnant women are more likely to have gingivitis or periodontitis. Apparently 40% of pregnant women may have periodontal disease.
There are two hypotheses that explain the increase in complications in this group: the first is that pathogens may cross the placental barrier reaching the amniotic fluid and fetal circulation, and the second, that the spread of endotoxins or inflammatory mediators may affect the development of the fetus or cause a miscarriage (3).
Prevention and treatment of periodontal disease
- At home, maintain proper oral hygiene, brushing your teeth at least twice a day (best after every meal), and once a day floss or use an interdental brush.
- Avoid eating sugary foods.
- Quitting smoking.
- Go to your dental checkups, as recommended by your dentist. In case of periodontal disease, a periodontist will assess your case and provide appropriate treatment (curettage, oral antibiotics…).
- Remember that brushing is sometimes not enough to remove the biofilm and bacteria located under the gums.
- In case of halitosis, painful, fragile, bleeding gums, or root exposure, do not hesitate, see your specialist.
- Try to manage your diabetes well with a good diet and exercise, and follow your doctors guidelines (1).
BIBLIOGRAPHY
(1) UpToDate : Overview of gingivitis and periodontitis in adults ( 1) (2) https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7035434/.
Voinescu I, Petre A, Burlibasa M, Oancea L.
Evidence of Connections Between Periodontitis and Ischemic Cardiac Disease – an Updated Systematic Review. Maedica (Buchar). 2019;14(4):384–390. doi:10.26574/maedica.2019.14.4.384
(3) https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6468093/pdf/main.pdf.
Bui FQ, Almeida-da-Silva CLC, Huynh B, et al. Association between periodontal pathogens and systemic disease. Biomed J. 2019;42(1):27–35. doi:10.1016/j.bj.2018.12.001

