The problem is not the lack of evidence, but the different way of assessing the scientific evidence of two groups: that of the scientist and that of the doctor. There are several types of studies that are fundamental in terms of the relationship between vitamin D and cancer.
Combining the different studies, the data suggest that having vitamin D in the range of 40-60ng/mL significantly reduces the risk of the onset of, and increases the survival from, many of the most common cancers. To maintain vitamin D in that range, doses between 2,000-5,000 IU per day may be required. It’s not about taking a certain amount, but rather about checking that we are effectively within the protective levels.
Dr. Iván Moreno – Neolife Medical Team
The scientific evidence can be of different kinds. With regard to vitamin D and cancer, there are several fundamental types.
The hypothesis for the relationship between UVB exposure – Vitamin D – cancer is almost 40 years old [Garland, 1980]. There are 5,293 publications with cancer and vitamin D or 25-hydroxy-vitamin D [25 (OH) D] in the title or abstract as recorded in pubmed.gov as of January 30th 2019. However, this hypothesis has not been widely accepted; in fact, since the publication of the results of the VITAL study (VITamin D and OmegA-3 TriaL [Manson, 2019], support for this relationship has been further curtailed. As we will discuss here, the problem is not the lack of evidence, but the different way of evaluating the scientific evidence of two groups: that of the scientist and that of the doctor.
Ecological studies.
The type of evidence used primarily to generate hypotheses is the geographical ecological study. In this approach, populations are defined by their geographic location and the rates of cancer that appear in both are compared, in addition to correlating them with the rates of sun exposure to UVB and other factors modifying the onset of cancer. This approach has identified up to 20 cancers in which there is an inverse correlation between the higher level of sun exposure and the lower mortality from these cancers in countries near the equator [Moukayed, Grant, 2013]. But since these types of studies can’t prove causality, but rather association, critics question-rightly-that perhaps other factors could explain the findings.
Observational studies.
Another type of studies are those known as “observational” studies. In these participants are usually included in cohorts or follow-up groups, with the levels of vitamin D being determined at the beginning and a follow-up over years to check for the possible appearance of tumors and a possible difference in the percentage of appearance between the groups according to different levels of vitamin D. These studies have found a strong inverse correlation between lower vitamin D values and greater appearance of colorectal cancer [Garland, Gorham, 2017], and less clearly but also related, with breast cancer [Grant, 2015], [Grant and Boucher, 2017]. The critics of these results argue that perhaps the relationship is the other way around: i.e. it’s the cancer that diminishes the vitamin D and the low vitamin the one that facilitates the cancer. There is no evidence that this happens in studies aimed at this, but it’s an argument that has gained force when it comes to explaining why, in some clinical trials in which vitamin D was given, the appearance of tumors was not reduced [Autier, 2017].
Studies of biological mechanisms.
A third type of study is the one that seeks to discover what in science is called “biological plausibility”, i.e. discovering the specific mechanism by which vitamin D may reduce the risk of dying from cancer . These mechanisms are well known to date, and can be grouped into those that reduce incidence, angiogenesis and metastatic spread [Moukayed, Grant, 2013], [Moukayed, Grant, 2017].
Genetic studies.
A fourth type of study involves using the data provided by people who have a mutation in the genes that regulate vitamin D levels [Zheng et al. 2017]. The advantage is that diet or sun exposure doesn’t interfere with these studies, so the possible causal relationship could end up being clearer. Unfortunately, mutations have very little effect on the levels of vitamin D, and would thus require large numbers of people with mutations that are in themselves already infrequent. There are several studies but no conclusive results, probably related to the insufficient strength of the studies for the reasons already described [Ong, 2018].
Controlled and randomized clinical trials.
This is the type of clinical study most frequently used in medicine. Two similar groups, and an intervention that is done at random without the patients or the doctors knowing who is receiving the vitamin and who the placebo.
One of the most important limitations of these studies with vitamin D, unlike drugs, is that our body already has vitamin D in itself, and the improvement in levels (and therefore, the possible positive impact in reducing cancer) are not the same if we administer it to a person who had very low levels or higher ones. With this limitation in mind, it was already appreciated that the right way to conduct studies with vitamin D was to evaluate its previous levels [Heaney, 2014], [Grant et al. al., 2018] . With this idea in mind, we will evaluate the different studies to date.
The first clinical trial showing the benefits of supplementation with vitamin D in cancer prevention was carried out in 2007, where they compared the administration of vitamin D + calcium, calcium alone and placebo. In this study they found a 60% reduction in the appearance of cancer. Both the levels of vitamin D at the beginning and the supplementation with vitamin D proved to be a predictor of the appearance of cancer. [Lappe, 2007].
The second study that showed benefit was a reanalysis of data from an extensive study in women, the Women’s Health Initiative. In a group of 15,000 women, those who hadn’t been taking calcium/vitamin D previously (and with low levels), were given calcium and vitamin D supplements (43% of all the women). The results showed a statistically significant reduction of total and breast cancer of around 14-20%. [Bolland, 2011].
The third major study that showed the benefit of vitamin D was conducted in 2017. In this study, the population was slightly overweight and had an average vitamin D level of 33ng/mL. 2,000 IU of vitamin D was administered with calcium or placebo. The group with vitamin D had an incidence of cancer of 4%, and the group with placebo of 6%, although they were not statistically significant differences. In an in-depth analysis, it was found that women who had indeed improved their levels from under 30 to 30-55ng/dL had reduced the incidence of cancer by 35%. It’s not as important how much vitamin D we give, but if we actually manage to improve the patients’ levels [Lappe, 2017].
The most recent study on vitamin D and cancer was the VITAL study (VITamin D and omega-3 TriaL [Manson, 2019]. This study had more than 25,000 patients, half of which received 2,000 IU of vitamin D and the other half received a placebo.
After a follow-up of 5.3 years, the study showed the appearance of cancer in 1617 participants, 793 with vitamin D and 824 with placebo, a difference that was not statistically significant. The conclusion communicated was that there is no difference in the appearance of cancer with vitamin D. The policy of the journal that published the VITAL study (The New England Journal of Medicine) is understandable in that it only publishes one major result from each study. What’s not so understandable is that the rest of the results that are statistically significant and very relevant in order to understand the role of vitamin D have not been communicated, specifically:
- The group with vitamin D had a 17% lower mortality rate from dying from cancer, which was higher (25%) if the cancers detected in the first two years were excluded (i.e. being understood that they were already there before the start of the study).
- For those who were overweight, the risk of invasive cancer was 14% lower, and for those who were not overweight 26% lower (a dose of 2,000 IU has a greater impact on the blood levels of vitamin D in a person with less weight).
Unfortunately, most of the general media and even the medical media only extract information from the abstract of the study (a brief summary that is included in each article), and have stopped reporting the benefits of vitamin D.
The baseline values (before treatment) were 28ng/mL in men and 32ng/mL in women.
Another factor that has contributed to the error when analyzing the results, is that the VITAL study was designed before the importance of measuring the levels of vitamin D prior to beginning the study was corroborated. The baseline values of 25,000 people were estimated by measuring only the levels in 395 males and 441 females. This was a missed opportunity to assess the hypothesis that vitamin D effectively protects against cancer in those people in whom the values do increase significantly.
Another error in the study was that at the time of its design a possible toxicity of vitamin D at high doses was raised, which although later proven not to be the case, led the directors of the study to use intermediate doses of vitamin D (2,000 IU). ) instead of the 4,000 that other previous studies considered beneficial [Ross, 2011] [Grant, 2016].
The association GrassrootsHealth.net has taken the initiative to study the effect based on the previous levels and those obtained after the supplementation with vitamin D. They have confirmed strong and statistically significant reductions in cancer risk (67%) when comparing levels greater than 40ng/dL with levels below 20ng/dL [McDonnell, 2016]. In a second, larger study, they found an 80% reduction in breast cancer with levels greater than 60ng/dL versus those under 20ng/dL [McDonnell, 2018].
Discussion
Reviewing the literature, the first ecological studies were based primarily on death rates for cancer, in which the impact of vitamin D is greater than on the rates of appearance of a new cancer.
However, on combining the different studies the data suggest that having vitamin D in the range of 40-60ng/mL significantly reduces the risk of the onset of, and increases the survival from, many of the most common cancers.
To maintain vitamin D within this range, doses between 2,000-5,000 IU per day may be required, depending on many factors. As the studies have confirmed, it’s not about taking a certain amount, but rather about checking that we are effectively within the protective levels.
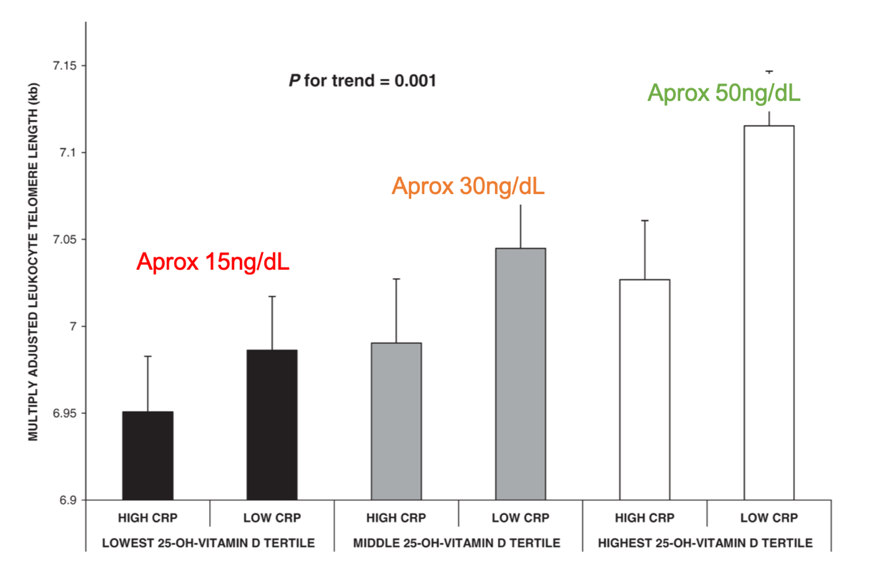
Apart from cancer, vitamin D has many other protective roles at the immune level, in bone protection and even in telomere shortening. Our genetic aging is lower if vitamin D levels are between 50 and 80ng/dL
Both biologists and doctors defend the need to have a scientific approach, considering the wide range of available evidence. For example, by following Hill’s criteria to demonstrate causality, the relationship between vitamin D and cancer prevention satisfies these [Grant, 2009 ; Mohr, 2012]. Far from falling into conspiracy theories that explain the lack of acceptance by the medical community of the proven benefits of vitamin D, which we can find in some forums suggesting that “medicine benefits from keeping us ill”, there are other causes that explain this resistance .
- Physicians are accustomed to analyzing the results of the effect of drugs in clinical trials. The problem is that the effect of vitamins and other essential nutrients can’t be analyzed in the same way. They are substances and nutrients that our body already has, and the design of the studies and their interpretation needs to be different.
- Unfortunately, medical training doesn’t usually go deeply into nutrition and into the relevance of micronutrients.
- Time is scarce when attempting to be constantly up to date in medicine, so doctors often fall into the mistake of reading only the abstracts of the studies without being able to analyze the results in detail. In cases such as the VITAL study, they give us only a partial view of the topic.
- In this age of excess information, we’re accustomed to receiving insistent information through the drug companies’ usual channels: a lot of repetition, visits by medical representatives, conferences, talks by experts in the subject, etc. This type of dissemination requires a lot of investment, which isn’t possible when they’re not drugs but vitamins and nutrients.
So there are a whole series of reasons why this disagreement exists, and a solution to the question of vitamin D and cancer that will have to come sooner or later: a well-performed study with measurement of levels before and after supplementation with good doses of vitamin D, increasing them if necessary until protective levels (50-80ng/dL) are achieved.
Meanwhile, and in light of the results, at Neolife we recommend supplementing with a dose that can be personalized, in order to achieve good levels that protect us adequately.
BIBLIOGRAPHY
(1) Autier P, Mullie P, Macacu A, Dragomir M et al. (2017) Effect of vitamin D supplementation on non-skeletal disorders: a systematic review of meta-analyses and randomised trials.Lancet Diabetes Endocrinol. 5:986-1004. https://www.ncbi.nlm.nih.gov/pubmed/29102433
(2) Bolland MJ, Grey A, Gamble GD, Reid IR. (2011) Calcium and vitamin D supplements and health outcomes: a reanalysis of the Women’s Health Initiative (WHI) limited-access data set.Am J Clin Nutr. 94:1144-1149. https://www.ncbi.nlm.nih.gov/pubmed/21880848
(3) Garland CF, Garland FC. (1980) Do sunlight and vitamin D reduce the likelihood of colon cancer? Int J Epidemiol. 9:227-231. https://www.ncbi.nlm.nih.gov/pubmed/7440046
(4) Garland CF, Gorham ED. (2017) Dose-response of serum 25-hydroxyvitamin D in association with risk of colorectal cancer: A meta-analysis. J Steroid Biochem Mol Biol. 168:1-8. https://www.ncbi.nlm.nih.gov/pubmed/27993551
(5) Grant WB, Boucher BJ. (2017) Randomized controlled trials of vitamin D and cancer incidence: A modeling study. PLoS One. 12(5):e0176448. https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0176448
(6) Grant WB, Boucher BJ, Bhattoa HP, Lahore H. (2018) Why vitamin D clinical trials should be based on 25-hydroxyvitamin D concentrations.J Steroid Biochem Mol Biol.177:266-269. https://www.ncbi.nlm.nih.gov/pubmed/28842142
(7) Grant WB, Karras SN, Bischoff-Ferrari HA, Annweiler C, Boucher BJ, Juzeniene A, Garland CF, Holick MF. (2016) Do studies reporting ‘U’-shaped serum 25-hydroxyvitamin D–health outcome relationships reflect adverse effects? Dermato-Endocrinology. 8: e1187349. https://www.ncbi.nlm.nih.gov/pubmed/27489574
(8) Grant WB. (2009) How strong is the evidence that solar ultraviolet B and vitamin D reduce the risk of cancer? An examination using Hill’s criteria for causality. Dermatoendocrinol. 1(1):17-24. https://www.ncbi.nlm.nih.gov/pubmed/20046584
(9) Grant WB. (2015) 25-Hydroxyvitamin D and breast cancer, colorectal cancer, and colorectal adenomas: case-control versus nested case-control studies, Anticancer Res. 35:1153-1160. https://www.ncbi.nlm.nih.gov/pubmed/25667506
(10) Heaney RP. (2014) Guidelines for optimizing design and analysis of clinical studies of nutrient effects. Nutr Rev. 72:48-54. https://www.ncbi.nlm.nih.gov/pubmed/24330136
(11) Lappe JM, Travers-Gustafson D, Davies KM, Recker RR, Heaney RP. (2007) Vitamin D and calcium supplementation reduces cancer risk: results of a randomized trial.Am J Clin Nutr. 85:1586-1591. https://www.ncbi.nlm.nih.gov/pubmed/17556697
(12) Lappe J, Watson P, Travers-Gustafson D, Recker R et al.(2017) Effect of Vitamin D and calcium supplementation on cancer incidence in older women: A randomized clinical trial.JAMA. 317:1234-1243. https://www.ncbi.nlm.nih.gov/pubmed/28350929
(13) Manson JE, Bassuk SS, Lee IM, Cook NR et al. (2012) The VITamin D and OmegA-3 TriaL (VITAL): rationale and design of a large randomized controlled trial of vitamin D and marine omega-3 fatty acid supplements for the primary prevention of cancer and cardiovascular disease.Contemp Clin Trials. 33:159-171. https://www.ncbi.nlm.nih.gov/pubmed/21986389
(14) Manson JE, Cook NR, Lee IM, Christen W et al. VITAL Research Group. (2019) Vitamin D Supplements and Prevention of Cancer and Cardiovascular Disease.N Engl J Med. 380:33-44. https://www.ncbi.nlm.nih.gov/pubmed/30415629
(15) McDonnell SL, Baggerly C, French CB, Baggerly LL, Garland CF, Gorham ED, Lappe JM, Heaney RP. (2016)Serum 25-Hydroxyvitamin D Concentrations =40ng/ml Are Associated with >65% Lower Cancer Risk: Pooled Analysis of Randomized Trial and Prospective Cohort Study.PLoS One. 11(4):e0152441. https://www.ncbi.nlm.nih.gov/pubmed/27049526
(16) McDonnell SL, Baggerly CA, French CB, Baggerly LL et al. (2018) Breast cancer risk markedly lower with serum 25-hydroxyvitamin D concentrations =60 vs < 20ng/ml (150 vs 50nmol/L): Pooled analysis of two randomized trials and a prospective cohort.PLoS One. 13(6):e0199265. https://www.ncbi.nlm.nih.gov/pubmed/29906273
(17) Mohr SB, Gorham ED, Alcaraz JE, Kane CI et al. (2012) Does the evidence for an inverse relationship between serum vitamin D status and breast cancer risk satisfy the Hill criteria?Dermatoendocrinol. 4(2):152-7. https://www.ncbi.nlm.nih.gov/pubmed/22928071
(18) Moukayed M, Grant WB. (2013) Molecular link between vitamin D and cancer prevention. Nutrients. 5:3993-4023. https://www.ncbi.nlm.nih.gov/pubmed/24084056
(19) Moukayed M, Grant WB. (2017) The roles of UVB and vitamin D in reducing risk of cancer incidence and mortality: a review of the epidemiology, clinical trials, and mechanisms. Rev Endocr Metab Disord. 18:167-182. https://www.ncbi.nlm.nih.gov/pubmed/28213657
(20) Ong JS, Gharahkhani P, An J, Law MH, Whiteman DC, Neale RE, MacGregor S. (2018) Vitamin D and overall cancer risk and cancer mortality: a Mendelian randomization study.Hum Mol Genet. 27:4315-4322. https://www.ncbi.nlm.nih.gov/pubmed/30508204
(21) Ross AC, Manson JE, Abrams SA, Aloia JF. (2011) The 2011 report on dietary reference intakes for calcium and vitamin D from the Institute of Medicine: what clinicians need to know.J Clin Endocrinol Metab. 96:53-58. https://www.ncbi.nlm.nih.gov/pubmed/21118827
(22) Zheng J, Baird D, Borges MC, Bowden J. (2017) Recent Developments in Mendelian Randomization Studies. Curr Epidemiol Rep. 4:330-345. https://www.ncbi.nlm.nih.gov/pubmed/29226067
(23) Richards JB, Valdes AM, Gardner JP, Paximadas D, Kimura M, Nessa A, et al. Higher serum vitamin D concentrations are associated with longer leukocyte telomere length in women. The American Journal of Clinical Nutrition. 2007 Nov;86(5):1420–5. https://www.ncbi.nlm.nih.gov/pubmed/17991655

